There are several common types of advanced wound care treatments available, each designed to promote healing and manage complex wounds effectively. Here are some of the most widely used options:
1. Negative Pressure Wound Therapy (NPWT): This involves using a vacuum dressing to promote healing by applying negative pressure to the wound, which helps to remove excess fluid and increase blood flow.
2. Hydrocolloid Dressings: These are moisture-retentive dressings that provide a moist environment, promoting healing while protecting the wound from external contaminants.
3. Alginate Dressings: Made from seaweed, these dressings are highly absorbent and ideal for wounds with significant exudate. They help to maintain a moist environment and promote healing.
4. Foam Dressings: These dressings are soft and absorbent, providing cushioning and protection for wounds while managing fluid levels.
5. Graft and Flap Surgery: For more severe wounds, surgical options such as skin grafts (transplanting skin from another area) or flap surgery (moving tissue from one area to another) may be necessary.
6. Biologic Dressings: These include products made from human or animal tissue that can help to promote healing and reduce infection.
7. Cellular and Tissue-based Products: These advanced therapies include stem cell treatments and growth factor therapies to enhance the body’s natural healing processes.
8. Antimicrobial Dressings: These dressings contain agents that help to prevent or treat infection, particularly in chronic wounds.
9. Compression Therapy: Often used for venous ulcers, this treatment helps improve circulation and reduce swelling through the application of pressure.
10. Oxygen Therapy: Hyperbaric oxygen therapy (HBOT) involves breathing pure oxygen in a pressurized room, which can significantly enhance wound healing by increasing oxygen delivery to tissues.
These treatments can be used alone or in combination, depending on the specific needs of the patient and the nature of the wound. It’s important to work with a healthcare professional to determine the most appropriate treatment plan.
The choice of treatment for complex wounds is influenced by a variety of factors, including:
1. Wound Type and Severity: The specific characteristics of the wound, such as its size, depth, location, and whether it is acute or chronic, play a significant role in determining the appropriate treatment.
2. Underlying Health Conditions: Patients with conditions like diabetes, vascular disease, or immune deficiencies may require specialized treatment approaches to address their unique healing challenges.
3. Infection Status: The presence of infection can dictate the choice of dressings and therapies. Antimicrobial treatments may be necessary if an infection is present.
4. Exudate Levels: The amount of fluid produced by the wound affects dressing selection. High-exudate wounds may require absorbent dressings, while low-exudate wounds might benefit from moisture-retentive options.
5. Patient’s Age and Overall Health: Age, nutritional status, and comorbidities can influence healing capacity and affect treatment options.
6. Patient Preferences: Involving the patient in the treatment decision-making process is crucial. Preferences regarding treatment type, frequency of care, and lifestyle considerations can impact the chosen approach.
7. Healing Goals: The desired outcome, such as complete closure of the wound or management of symptoms, will guide the treatment plan.
8. Cost and Accessibility: Financial considerations and access to certain treatments or specialized care can also influence decisions regarding wound management.
9. Healthcare Provider Expertise: The experience and training of healthcare providers can affect the choice of treatment, as some may have more familiarity with specific advanced therapies.
10. Response to Previous Treatments: The effectiveness of any treatments already attempted can inform the next steps in the care plan, guiding the selection of alternative therapies if initial approaches were unsuccessful.
By considering these factors, healthcare providers can develop a comprehensive and individualized treatment plan that meets the specific needs of each patient with complex wounds.
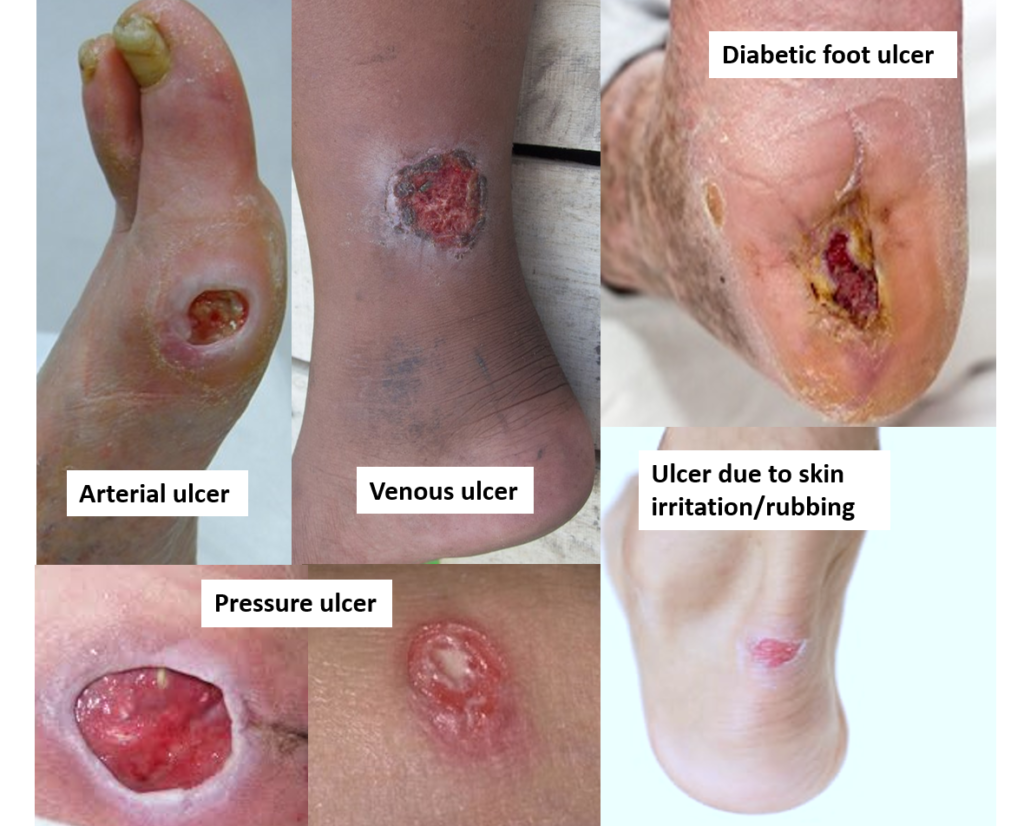
Complex wounds can vary widely in their causes and characteristics, but some of the most common types include:
1. Diabetic Ulcers: These are chronic wounds that occur as a result of diabetes, often on the feet. They develop due to nerve damage, poor circulation, and pressure, making them difficult to heal.
2. Venous Ulcers: These are caused by poor blood flow in the veins, typically occurring in the lower legs. They often result from conditions like chronic venous insufficiency and can be slow to heal.
3. Arterial Ulcers: These occur due to inadequate blood flow to the tissues, often resulting from peripheral artery disease. They are typically found on the feet or toes and can be quite painful.
4. Pressure Ulcers (Bedsores): These wounds develop when there is prolonged pressure on the skin, commonly affecting individuals who are immobile. They can range from mild redness to deep tissue damage.
5. Surgical Wounds: Complications can arise from surgical sites, leading to infections or dehiscence (wound reopening). These wounds may require advanced care if healing is impaired.
6. Traumatic Wounds: These include wounds resulting from accidents, falls, or injuries, such as lacerations or puncture wounds. When complicated by infection or other factors, they can become complex.
7. Burn Wounds: Severe burns can lead to complex wounds that require extensive care. Depending on the depth and extent of the burn, healing can be prolonged and may involve grafting.
8. Skin Tears: Often seen in older adults or those with fragile skin, skin tears occur when the skin is pulled or sheared. They can become complex if not managed properly.
9. Infected Wounds: Any wound that becomes infected can develop into a complex wound, requiring advanced treatment to address the infection and promote healing.
10. Non-healing Wounds: Wounds that do not respond to standard treatments over time may be classified as complex, necessitating specialized interventions to address underlying issues.
Each type of complex wound presents unique challenges and requires a tailored approach to treatment to promote healing and prevent complications.
he most effective treatments for venous ulcers focus on improving blood flow, promoting healing, and managing symptoms. Here are some of the key treatments:
1. Compression Therapy: This is the cornerstone of venous ulcer treatment. Compression bandages or stockings help improve venous return, reduce swelling, and promote healing by applying consistent pressure to the affected area.
2. Wound Care: Proper wound management is crucial. This includes regular cleaning, debridement (removing dead tissue), and applying appropriate dressings to maintain a moist environment and protect the wound from infection.
3. Elevation: Elevating the affected limb can help reduce swelling and improve venous drainage, especially when combined with compression therapy.
4. Topical Treatments: Depending on the condition of the ulcer, healthcare providers may use topical agents like antimicrobial ointments or growth factor dressings to promote healing and prevent infection.
5. Surgical Options: In some cases, surgical interventions may be necessary to address underlying venous insufficiency. Procedures can include vein stripping, endovenous laser treatment, or sclerotherapy to close off problematic veins.
6. Lifestyle Modifications: Encouraging patients to adopt a healthy lifestyle can significantly impact healing. This includes maintaining a healthy weight, exercising to improve circulation, and avoiding prolonged standing or sitting.
7. Medications: In certain cases, medications may be prescribed to manage pain, inflammation, or underlying conditions that contribute to poor healing.
8. Bioengineered Skin Substitutes: For chronic or non-healing venous ulcers, advanced treatments such as skin substitutes may be used to promote healing by providing a temporary barrier and promoting tissue regeneration.
9. Nutritional Support: Ensuring adequate nutrition, particularly protein and vitamins, is essential for wound healing. Nutritional assessment and supplementation may be recommended.
10. Patient Education: Educating patients about their condition, the importance of adherence to treatment, and recognizing signs of complications is vital for effective management and prevention of recurrence.
A combination of these treatments, tailored to the individual’s needs and the specific characteristics of the ulcer, typically yields the best outcomes in managing venous ulcers. Regular follow-up with healthcare providers is essential to monitor progress and make necessary adjustments to the treatment plan.
Nutrition plays a critical role in overall wound healing by providing the essential nutrients that support the body’s repair processes. Here are several ways in which nutrition impacts wound healing:
1. Protein: Protein is vital for tissue repair and regeneration. It provides the building blocks (amino acids) necessary for collagen synthesis, which is crucial for wound healing. Insufficient protein intake can lead to delayed healing and increased risk of infection.
2. Calories: Adequate caloric intake is necessary to meet the increased energy demands of the body during the healing process. A calorie deficit can hinder recovery and lead to muscle wasting and other complications.
3. Vitamins:
– Vitamin C: Essential for collagen synthesis and immune function, vitamin C helps in the formation of new tissue and enhances wound healing.
– Vitamin A: Important for epithelial cell differentiation and immune response, vitamin A supports skin health and aids in the healing of wounds.
– Vitamin E: Acts as an antioxidant, helping to protect cells from damage and supporting the healing process.
4. Minerals:
– Zinc: Plays a crucial role in cell division, protein synthesis, and immune function. Zinc deficiency can lead to prolonged healing times and increased risk of infection.
– Copper: Involved in collagen formation and the functioning of enzymes important for wound healing.
5. Hydration: Adequate fluid intake is essential for maintaining skin hydration, promoting circulation, and supporting overall metabolic processes. Dehydration can impair healing and increase the risk of complications.
6. Fatty Acids: Omega-3 fatty acids, found in fish oil and certain plant oils, can help reduce inflammation and promote a more favorable healing environment.
7. Antioxidants: Foods rich in antioxidants help combat oxidative stress and support the immune system, which is crucial for preventing infections and promoting healing.
8. Dietary Fiber: A diet high in fiber supports digestive health, which is important for overall well-being and nutrient absorption.
9. Individualized Nutrition Plans: Specific dietary needs may vary based on the type and severity of the wound, the patient’s overall health, and any underlying conditions (e.g., diabetes). Personalized nutrition plans can optimize healing.
10. Impact of Malnutrition: Malnutrition can significantly delay wound healing, increase the risk of infections, and lead to complications. Identifying and addressing nutritional deficiencies is essential for effective wound care.
In summary, a well-balanced diet rich in essential nutrients is vital for promoting effective wound healing. Healthcare providers often assess nutritional status and may recommend dietary changes or supplements as part of a comprehensive wound care plan.
The most effective treatments for venous ulcers focus on improving blood flow, promoting healing, and managing symptoms. Here are some of the key treatments:
1. Compression Therapy: This is the cornerstone of venous ulcer treatment. Compression bandages or stockings help improve venous return, reduce swelling, and promote healing by applying consistent pressure to the affected area.
2. Wound Care: Proper wound management is crucial. This includes regular cleaning, debridement (removing dead tissue), and applying appropriate dressings to maintain a moist environment and protect the wound from infection.
3. Elevation: Elevating the affected limb can help reduce swelling and improve venous drainage, especially when combined with compression therapy.
4. Topical Treatments: Depending on the condition of the ulcer, healthcare providers may use topical agents like antimicrobial ointments or growth factor dressings to promote healing and prevent infection.
5. Surgical Options: In some cases, surgical interventions may be necessary to address underlying venous insufficiency. Procedures can include vein stripping, endovenous laser treatment, or sclerotherapy to close off problematic veins.
6. Lifestyle Modifications: Encouraging patients to adopt a healthy lifestyle can significantly impact healing. This includes maintaining a healthy weight, exercising to improve circulation, and avoiding prolonged standing or sitting.
7. Medications: In certain cases, medications may be prescribed to manage pain, inflammation, or underlying conditions that contribute to poor healing.
8. Bioengineered Skin Substitutes: For chronic or non-healing venous ulcers, advanced treatments such as skin substitutes may be used to promote healing by providing a temporary barrier and promoting tissue regeneration.
9. Nutritional Support: Ensuring adequate nutrition, particularly protein and vitamins, is essential for wound healing. Nutritional assessment and supplementation may be recommended.
10. Patient Education: Educating patients about their condition, the importance of adherence to treatment, and recognizing signs of complications is vital for effective management and prevention of recurrence.
A combination of these treatments, tailored to the individual’s needs and the specific characteristics of the ulcer, typically yields the best outcomes in managing venous ulcers. Regular follow-up with healthcare providers is essential to monitor progress and make necessary adjustments to the treatment plan.